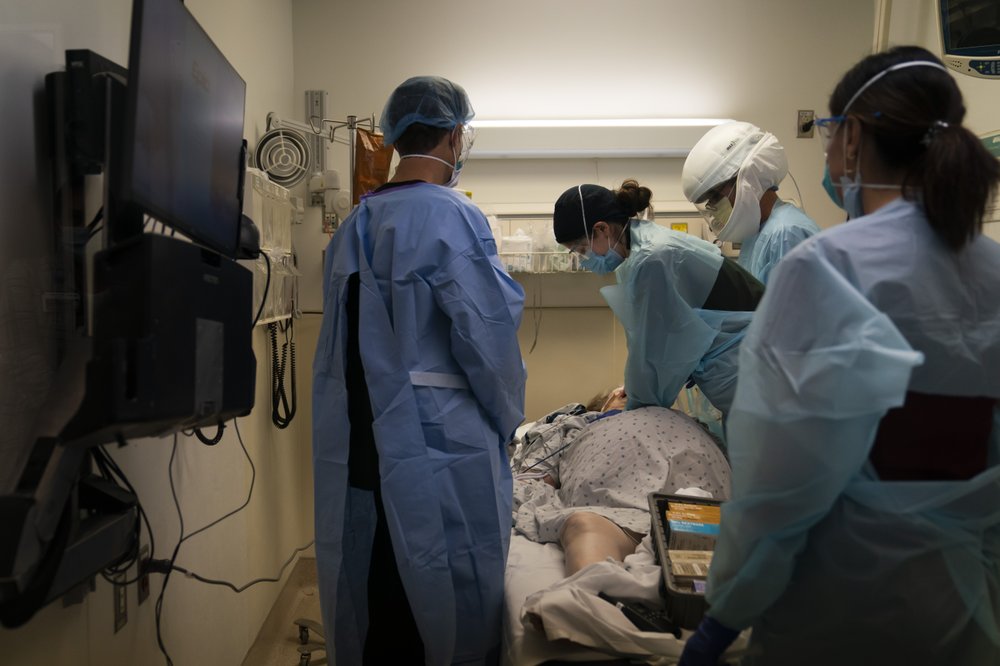
LONDON, United Kingdom (AFP)— Hospital chiefs in England raced to secure hospital beds on Thursday as the surge in coronavirus cases risked overwhelming the system, healthcare providers and medics said.
A leaked briefing suggested that even in a relatively positive scenario, London’s hospitals could be beyond capacity in less than two weeks.
The UK on Thursday recorded another 1,162 deaths within 28 days of a positive test — the second highest toll since the peak of the first wave in April last year.
There were more than 52,000 new cases in 24 hours, taking the overall number of infections to nearly 2.9 million.
Cases are growing quickly outside southeast England, where clusters of a new highly infectious strain of the virus were first identified.
Over 30,000 people were in UK hospitals with the virus, more than at the peak of the first wave, heaping pressures on healthcare staff.
“Staff are exhausted,” said Lindsey Izard, matron of the general intensive care unit at St George’s Hospital in London.
“The worry is that we haven’t probably reached the peak yet.”
The sharp rise has forced hospital bosses to consider shifting some inpatients to beds in nursing homes or care homes, said the head of NHS Providers, which represents hospitals in England.
“We’ve seen 5,000 new patients in hospital beds with COVID-19 over the past week — that’s 10 full hospitals’ worth of COVID patients… so it’s a really big challenge,” Chris Hopson told BBC radio.
Hospital chiefs “know there is some spare capacity in the care and nursing home sector and they’re in the middle of conversation with care and nursing home colleagues to see if they can access that capacity”, he added.
In the face of the mounting crisis, the UK’s Department of Health and Social Care on Thursday announced two potentially “live-saving” COVID treatments would be made available for patients in intensive care.
The two drugs — tocilizumab and sarilumab — have been shown to reduce risk of death by 24 percent for critically ill patients and cut the time spent in intensive care by up to 10 days, the government said.
Health Secretary Matt Hancock called the deployment of the drugs a “landmark development”, saying the treatments, normally used for rheumatoid arthritis, would save hundreds of lives.
England entered a strict lockdown on Tuesday with schools and non-essential shops closed for at least six weeks after previous measures failed to halt a steep rise in cases.
- ‘Take lockdown seriously’ –
Britain has seen more than 78,500 deaths in the outbreak and is banking on the roll-out of the Pfizer/BioNTech and Oxford/AstraZeneca vaccines to halt the spread of the virus.
More than 1.3 million have already received jabs. The government aims to have inoculated 13 million of the most vulnerable groups by mid-February.
Speaking to a parliamentary select committee, Hancock said he expected hospitalisation levels and COVID deaths to fall as the vaccine programme continued.
“The number of deaths in this country will fall for any given number of cases once the vaccine is rolled out to the vulnerable groups,” he said.
HSJ, a website for healthcare professionals, on Wednesday leaked a briefing by the head of NHS London, Vin Diwakar, saying the capital could be short of nearly 1,500 beds for general and acute patients by January 19.
In the worst-case scenario, the shortfall could be 4,400 beds, it said.
Hospital capacity is at risk unless people knuckle down to anti-virus lockdown rules, said Rupert Pearse, a professor of intensive care medicine at Queen Mary, University of London, who works at the Royal London Hospital.
Asked by the BBC whether he believed the NHS could be overwhelmed in two weeks, he said: “I never thought in my entire career that I would say something like this but yes, I do.
“Unless we take the lockdown seriously the impact on healthcare for the whole country could be catastrophic and I don’t say those words lightly,” he added.
Source: Jamaica Observer